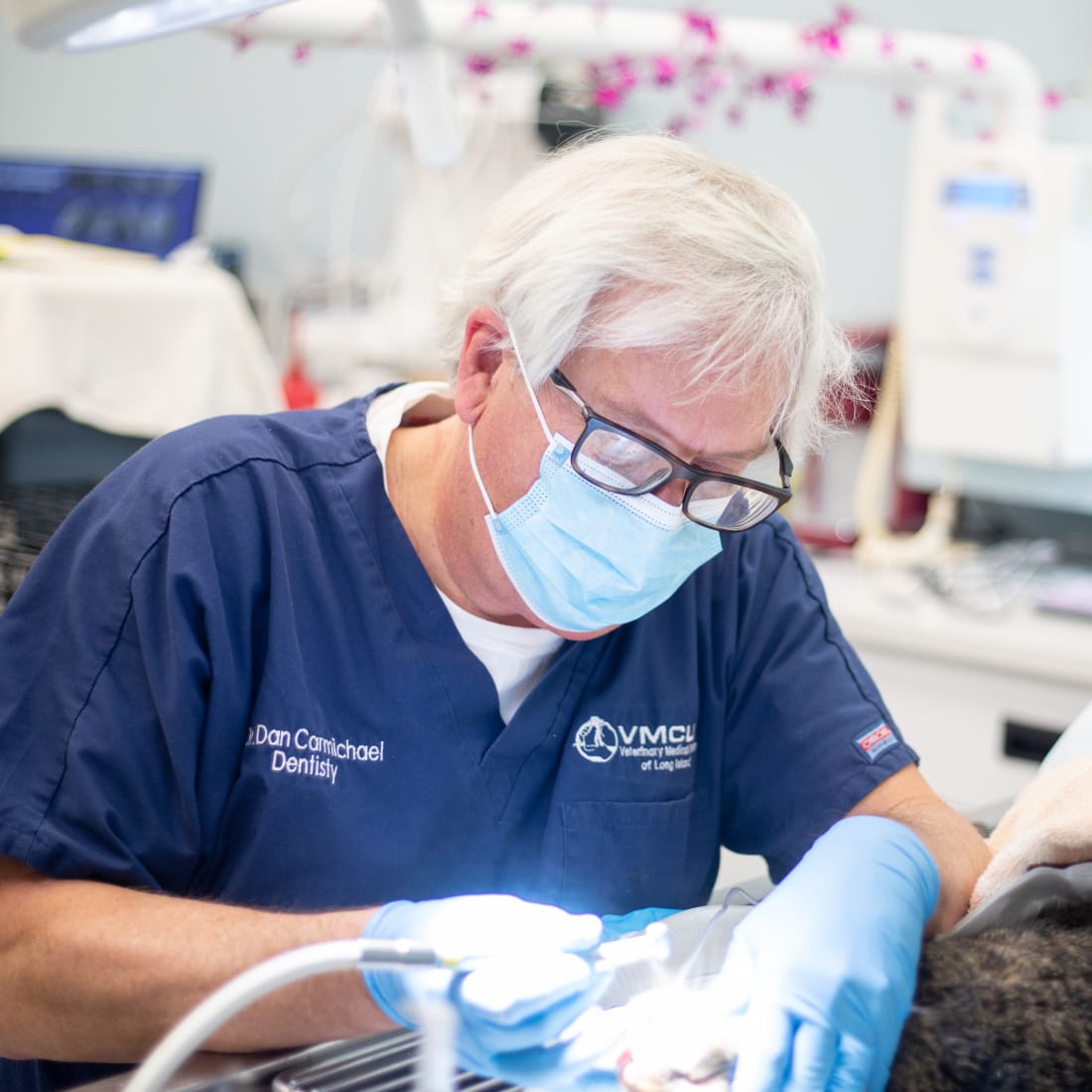
Comprehensive Veterinary Dental Care
Dental disease is the most common disease of both dogs and cats. Over 50% of cats and 85% of dogs over the age of three require professional dental treatment.
When left untreated, dental issues can lead to complications that may require further veterinary care. Our dental specialists offer the services needed to prevent and treat a number of dental concerns.
Our veterinary dental team has extensive experience which helps them to address and manage your companion's oral health. From dental evaluations to specialized services such as restorative care and endodontics, your pet is in good hands.
We believe in communication and patient education and will keep you informed throughout your dog or cat's dental treatment, discussing our findings and any recommendations we have with you.
Veterinary Dental Specialists
At Veterinary Medical Center of Long Island, our experienced dental team consists of board-certified dental specialists and veterinary technicians who are highly trained and work cohesively to provide routine care and specialized services for your pet.
Specialized Dental Services for Pets
Our veterinary dentist provides specialized dental care for pets on Long Island including the following dental services:
- Annual dental exam
- Periodontics
- Oral surgery (extractions, biopsies, tumor removal)
- Prosthodontics (crown therapy)
- Restorative dentistry
- Endodontics (root canals)
- Orthodontics (bite correction)
- Fracture repair
- Recommendations for oral health care at home
Dental Procedures & Anesthesia
Our dental specialists use the latest equipment in all dental procedures from routine cleanings to restorative surgery.
For patient comfort and safety our dental suite includes heart and blood pressure monitors, patient warming systems, and state-of-the-art Sevoflurane® anesthesia equipment.
Whether your pet is visiting us for an exam and cleaning or undergoing dental surgery, anesthesia allows your veterinarian to perform dental procedures with minimal stress and pain for the patient.
Rest assured, before going under anesthesia, your pet will always be evaluated first to ensure it is safe for them. Your pet will also be continuously monitored while under anesthesia.
